"This is a preliminary report of work that has not been certified by peer review. This should not be relied on to guide clinical practice or health-related behavior and should not be reported in news media as established information."Ran across a link to this recent R&D paper (39 pg PDF) over at Naked Capitalism. Interesting, in light of my prior rants on lab QA issues.
ABSTRACT"Well-designed studies to elucidate the mechanisms and serological correlates of protective immunity will be crucial to guide rational clinical and public health policies."
Background
Serological tests are crucial tools for assessments of SARS-CoV-2 exposure, infection and potential immunity. Their appropriate use and interpretation require accurate assay performance data.
Method
We conducted an evaluation of 10 lateral flow assays (LFAs) and two ELISAs to detect anti SARS-CoV-2 antibodies. The specimen set comprised 130 plasma or serum samples from 80 symptomatic SARSCoV-2 RT-PCR-positive individuals; 108 pre-COVID-19 negative controls; and 52 recent samples from individuals who underwent respiratory viral testing but were not diagnosed with Coronavirus Disease 2019 (COVID-19). Samples were blinded and LFA results were interpreted by two independent readers, using a standardized intensity scoring system.
Results
Among specimens from SARS-CoV-2 RT-PCR-positive individuals, the percent seropositive increased with time interval, peaking at 81.8-100.0% in samples taken >20 days after symptom onset. Test specificity ranged from 84.3-100.0% in pre-COVID-19 specimens. Specificity was higher when weak LFA bands were considered negative, but this decreased sensitivity. IgM detection was more variable than IgG, and detection was highest when IgM and IgG results were combined. Agreement between ELISAs and LFAs ranged from 75.8-94.8%. No consistent cross-reactivity was observed.
Conclusion
Our evaluation showed heterogeneous assay performance. Reader training is key to reliable LFA performance, and can be tailored for survey goals. Informed use of serology will require evaluations covering the full spectrum of SARS-CoV-2 infections, from asymptomatic and mild infection to severe disease, and later convalescence. Well-designed studies to elucidate the mechanisms and serological correlates of protective immunity will be crucial to guide rational clinical and public health policies.
Important, vitally necessary work. This particular effort focuses on qualitative ("positive/negative") screens via which to detect the presence (or absence) of Novel Coronavirus antibodies--possible markers of immunity for those having been exposed to the pathogen (even if subsequently remaining asymptomatic).
Suffice it to observe again than bioassay accuracy does not come quickly or on the cheap (gotta love their poignantly euphemistic "heterogeneous assay performance" admission). Moreover, after a test method is validated and approved at the R&D level, ongoing vigilant QA remain necessary at the production bench level. Neither is that cheap. Concurrent best-practice minimization of false positives and false negatives (the "sensitivity" vs "specificity" thing) is no cakewalk.
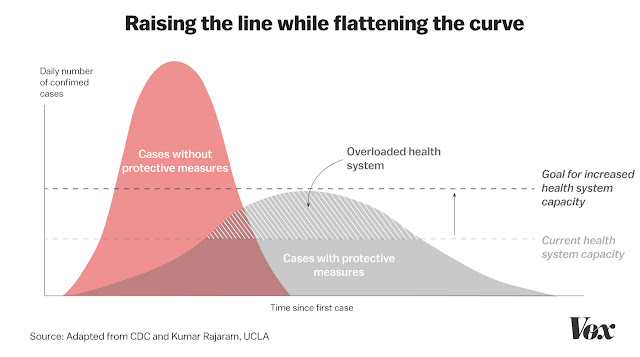
We remain seriously behind the curve on effective screening at scale for the current pandemic crisis.
STATnews article:
Many states are far short of Covid-19 testing levels needed for safe reopening, new analysis shows
More than half of U.S. states will have to significantly step up their Covid-19 testing to even consider starting to relax stay-at-home orders after May 1, according to a new analysis by Harvard researchers and STAT.UPDATE FROM SCIENTIFIC AMERICAN
The analysis shows that as the U.S. tries to move beyond its months-long coronavirus testing debacle — faulty tests, shortages of tests, and guidelines that excluded many people who should have been tested to mitigate the outbreak — it is at risk of fumbling the next challenge: testing enough people to determine which cities and states can safely reopen and stay open. Doing so will require the ability to catch reappearances of the coronavirus before it again spreads uncontrollably…
Scientists have long warned that the rate of emergence of new infectious diseases is accelerating—especially in developing countries where high densities of people and animals increasingly mingle and move about...POTUS TODAY
APR 28TH UPDATEPresident Trump: "The testing itself is going really well. No complaints." pic.twitter.com/dVSUWNOCiB— The Hill (@thehill) April 27, 2020
YASCHA MOUNK, associate professor at Johns Hopkins UniversityYeah. Interesting Atlantic article.
America is still behind on testing for COVID-19. Although Trump promised almost two months ago that anyone who wanted a test could get one, the U.S. has still conducted only about 5.4 million. The country needs to increase its testing rate at least threefold to reopen safely.
America is also behind on test and trace. Some countries, such as South Korea, now have robust systems in place to inform people that they have been exposed to the coronavirus, and need to self-isolate. But implementing such a system requires two things the United States sorely lacks: widespread trust in the government and a coordinated response from the White House.
In the absence of a federal strategy, some states, such as New York and Massachusetts, are trying to develop their own test-and-trace systems. But without help from Washington, they will likely lack both the resources to build a comprehensive system and the ability to persuade a large majority of their residents to sign up for an app that tracks their movements. Even if, against the odds, they should succeed in both these tasks, they face another obvious obstacle: Viruses don’t respect state lines.
If he were truly interested in limiting the damage to America’s economy, and opening up the country, Trump would be laser-focused on remedying these problems. Instead, the president has doubled down on culture wars and quack cures.
Early last week, Trump fanned the flames of the irresponsible protests against stay-at-home orders that are now being staged in cities across the country. A few days later, he vowed to “suspend immigration” to the United States. Then he suggested that scientists look into the possibility of injecting patients with bleach.
For all his blustering demands to get the country back to normal, the president is failing to take the steps that are required to reopen the economy without a horrific death toll. And for all the ingenuity shown by individual governors, the absence of a coordinated federal strategy may prove impossible to overcome…
A SAD DAY HERE
Two years ago today, my younger daughter Danielle succumbed to her severe pancreatic cancer, 20 years after we lost her elder sister Sissy to an unrelated cancer.
Sigh...
_____________
More to come...