This week the DC Carnival kicks off with two congressional hearings: CMS head Marilyn Tavenner appears before the Ways and Means Committee tomorrow, followed by Wednesday's Main Event Match between HHS Secretary Sebelius and the House Energy and Commerce Committee. I will be breaking out the popcorn for both of those. But, first...
The Power of Photoshop Compels Me.
Lifted the Susan Collins quote from this paper:
Kludgeocracy: The American Way of Policy
Steven M. Teles, Associate Professor of Political Science, Johns Hopkins University
December 2012
The last thirty years of American history have witnessed, at least rhetorically, a battle over the size of government.1 Yet that is not what the history books will say the next thirty years of American politics were about. With the frontiers of the state roughly fixed, the issues that will dominate American politics going forward will concern the complexity of government, rather than its sheer size....
...Martha Derthick shows that the confused joint administration of the flood protection system of New Orleans played a vital role in the system’s failure during Hurricane Katrina.6 Derthick quotes Sen. Susan Collins as having found that there was “confusion about the basic question of who is in charge of the levees,” an inherent problem given our pervasive, kludgey interweaving of federal and state responsibilities. Because administering programs through intergovernmental cooperation introduces pervasive coordination problems into even rather simple governmental functions, the odds that programs with shared rather than solo responsibility will have unintended consequences and sluggish administration are, inevitably, high.
Kludgeocracy is also a significant threat to the quality of our democracy. The complexity that makes so much of American public policy vexing and wasteful for ordinary citizens and governments, however, is also what makes it so easy for organized interests to profit off the state’s largesse...
The Causes of Kludgeocracy
The costs of kludgeocracy, therefore, are considerable. To do something about it, however, requires that we understand why American politics turns to kludgey solutions so regularly.
A condition as chronic as kludgeocracy is inherently multi-causal, but the key interlocking causes of kludgeocracy are the structure of American institutions, the desire to preserve the fiction of small government while also addressing public problems, and the emergence of a “kludge industry” that supplies a constant stream of complicated, roundabout solutions. I will address each in turn."administering programs through intergovernmental cooperation introduces pervasive coordination problems into even rather simple governmental functions."
We were all taught in school that American institutions were designed to constrain the growth of government. This is, of course, why those on the right tend to defend our founding institutional heritage, while many liberals as far back as the Progressive Era have voiced considerable skepticism. But there are reasons to be skeptical of the idea that federalism and the separation of powers limit the growth of government, since a huge pile of political science scholarship shows that when we look beyond spending and taxation and focus on policy tools that the United States has historically relied on more heavily, such as regulation, litigation, and tax expenditures, the activity of the American state is not starkly different than other industrial countries.
American institutions do, in fact, serve to constrain the most direct forms of government taxing and spending. But having done so, they do not dry up popular or special interest demands for government action, nor do they eliminate the desire of politicians to claim credit for new government activity. Public demand, when prevented from flowing directly, does not disappear. Instead, it spreads out in complicated, unpredictable ways...
Yeah, and add to that the myriad private sector players intextricably woven into the tapestry (e.g., the AHIP crowd), and the potential for adverse unintended consequences rises materially.
Speaking of private sector players (with a PPACA contract, to be sure), this is one of today's headlines.
Obamacare Websites Limited by Verizon Data Hub FailureThe wags are out in force, snarkily arguing that that the feds should simply have turned the entire PPACA HIX rollout to high-tech commerical vendors such as Amazon or Google.
By Alex Wayne - Oct 28, 2013 11:13 AM PT
The Obamacare data hub that routes applicant information to websites run by the federal government and 14 states resumed service after failing yesterday.
The data hub center, operated by Verizon Communications Inc. (VZ)’s Terremark unit, lost connectivity after workers tried to replace a broken networking component. As of 7 a.m. today New York time, the hub was “fully operational,” according to an e-mailed statement from Joanne Peters, a spokeswoman for the U.S. Health and Human Services Department...
Lordy.
__
OCTOBER 29TH UPDATE
CMS's Marilyn Tavernner testifies today. Also, note the little "in case you missed it" headline. MSNBC is all over that this morning.
President Obama repeatedly assured Americans that after the Affordable Care Act became law, people who liked their health insurance would be able to keep it. But millions of Americans are getting or are about to get cancellation letters for their health insurance under Obamacare, say experts, and the Obama administration has known that for at least three years.Buffeted at every turn. Gonna be an interesting week.
Four sources deeply involved in the Affordable Care Act tell NBC News that 50 to 75 percent of the 14 million consumers who buy their insurance individually can expect to receive a “cancellation” letter or the equivalent over the next year because their existing policies don’t meet the standards mandated by the new health care law. One expert predicts that number could reach as high as 80 percent. And all say that many of those forced to buy pricier new policies will experience “sticker shock.”...
While we await today's congressional hearing festivities...
BACK TO MEANINGFUL USE, BRIEFLY
What GAO FoundComplete PDF copy of the 50 page report here.
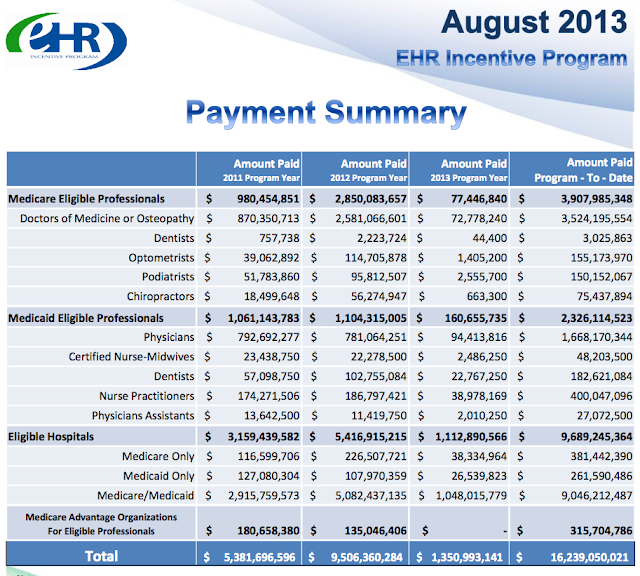
Hospitals and health care professionals, such as physicians, were awarded a total of approximately $6.3 billion in Medicare electronic health records (EHR) incentive payments for 2012, which is more than twice the $2.3 billion awarded to hospitals and professionals for 2011. Almost half of eligible hospitals and less than a third of eligible professionals received Medicare EHR incentive payments for 2012.
For 2012, the 2,291 hospitals that were awarded payments represent 48 percent of the eligible hospitals and an increase compared to 2011, when 777 hospitals, or 16 percent of those eligible, were awarded payments. Nationwide, 72 percent of hospitals were new to the program; that is, they were awarded an incentive payment for the first time. Participation varied among hospitals with certain characteristics. For example, acute care hospitals were nearly twice as likely as critical access hospitals to have been awarded an incentive payment for 2012. In addition, hospitals in rural areas were 3.1 times more likely to have been awarded an incentive payment for 2012 compared to 2011, a slightly greater increase than for hospitals overall.
Additionally, 183,712 professionals were awarded payments for 2012, which represents 31 percent of the eligible professionals and an increase compared to 2011, when 58,331 professionals, or 10 percent of those eligible, were awarded incentive payments.
Nationwide, 75 percent of professionals that were awarded an incentive payment for 2012 were new to the program. General practice physicians were 1.5 times more likely than specialty practice physicians to have been awarded an incentive payment for 2012. In addition, professionals with the lowest total amount of Medicare Part B charges were 3.3 times more likely to have been awarded an incentive payment for 2012 compared to 2011, which was a slightly greater increase than for professionals overall.
Why GAO Did This Study
Widespread use of health information technology, such as EHR, has the potential to improve the quality of care patients receive and reduce health care costs. The Health Information Technology for Economic and Clinical Health (HITECH) Act, enacted as part of the American Recovery and Reinvestment Act of 2009 (Recovery Act), among other things, provided funding for various activities intended to promote the adoption and meaningful use of certified EHR technology, including the Medicare and Medicaid EHR programs. Starting in 2011, these programs have provided incentive payments for hospitals and professionals that demonstrate meaningful use of certified EHR technology and meet other program requirements established by the Centers for Medicare & Medicaid Services (CMS). This report provides information on certain providers, including hospitals and professionals, that were awarded Medicare EHR incentive payments for 2011 and 2012. Using data from CMS and other government and private sources, GAO determined the number and percentage of eligible providers awarded Medicare incentive payments; determined the amount of Medicare EHR incentive payments awarded to providers; and examined the characteristics of providers that were awarded Medicare EHR incentive payments.
__
And, now...
POST-HEARING SUMMARY
Not much to say. About 10 minutes of partisan speechifying for every actual question posed to the witness (and with many of the adversarial questions coming from the Republican members being simply repetitive, banging away at the same point). Ms. Tavenner gave as good as she got. The Big Prize is tomorrow, when HHS Secretary Sebelius testifies before the House Energy and Commerce Committee.
Nice summary here.
Dem congressman to GOPer at Obamacare hearing: “Are you really serious!?”
Rep. Bill Pascrell absolutely loses it during a House hearing on Obamacare
BY ELIAS ISQUITH
While today’s Obamacare hearing may not have shed much light on the workings of the law, it did teach us this much: New Jersey Congressman Bill Pascrell likes to stand up when he yells at Republicans.
And during Tuesday’s hearing on Obamacare, that’s just what he did. First Pascrell pointed his finger at Republicans for their unwillingness to cooperate with the implementation of Obamacare, contrasting the GOP’s behavior over the past three years with that of the Democratic Party in the years following the passage of George W. Bush’s Medicare Part D.
“What did we do [after Medicare Part D passed]? We went back to our districts, and we told our seniors that although we voted no, we personally believe, and will work with the Bush administration, to make it work. That’s what we did!”
Pascrell then stood up and yelled at the Republican members of Congress attending the hearing, “And how many of you stood up to do that? None! Zero! Zero!”
Later in Pascrell’s harangue, the New Jersy congressman asked Republicans what they would say to those with preexisting conditions in the event that Obamacare was repealed. “What are you going to do about the approximately 17 million children with preexisting conditions who can no longer be denied health insurance coverage?” Pascrell said. “We want to go back and want to say you are no longer covered any longer — are you going to tell the parents of those kids?”...
___
WEDNESDAY OCT 30TH
Showtime. Sworn in under Oath, 18.USC.1001.
UNDERSTATEMENT OF THE DAY
__
Ranking Member Rep. Waxman, in his opening statement, asks the Republicans to stop hyperventilating.
No chance. Rep. Marsha Blackburn (R-TN) could not be more hostile right out of the gate.
Slate's John Dickerson writes
When healthcare.gov launched with the fanfare and success of a North Korean missile, the president insisted that Obamacare was more than a website. The website might be a mess, but the underlying product was sound. Now, it's Republicans who are using this exact phrase. Like the president, GOP leaders want people to focus on the larger law. You can fix a website, they say, but you can't improve the law.Another gem, from polizeros.com
What started as a website debacle is growing into a relitigation of the underlying operation. The Affordable Care Act passed with cracks and inconsistencies that are now re-emerging in the context of the website's bad launch. In some cases that simply gives Republicans new lines of attack. In others, like this argument over keeping your old health care, the failure of the site is weakening the administration's ability to engage in those old debates.
Federal CIO Steven VanRoekel spouts perky inanities about the wonderfulness of healthcare.gov and is so clueless about software development it makes my head hurt.
I present to you this gem of confusion.CNN's ANDERSON COOPER
“We should all be proud of the fact that something this complex, this integrated to legacy systems — and there are mainframes out there this thing hooks to — was done at Internet scale and taken online in this way. Just the fact that we have transactions moving between agencies using open data, using modular development, using technology in a way that moves really from a 19th and 20th Century government paper approach to an online approach is something we all should be proud of,” VanRoekel said.Oh my God, you mean the online healthcare.gov can actually talk to mainframes? This staggering new development has only been going on since, oh, shortly after the birth of the Internet. Modular development of software, which he thinks is cutting edge, has been around for 50 years or so. I’ve no clue what he means by ‘open data.’ I suspect he means ‘open source.’ For the head techie of the US government to not even get that basic concept and jargon correct in deeply troubling. And ‘Internet scale” is…?
"Could you imagine the [Obama] campaign, if their website had been like this during the campaign? You think they would have stood for that?"WHO WROTE THIS?
"The cost of fixing an error in an application increases as much as ten times if it has to be rectified in a production environment. The risks associated with inadequate testing, and consequently with insufficient quality, are rising, particularly with the increasing complexity of multiple and inter-dependent applications. Testing is a key phase of any project, and if conducted the right way, gives a business owner an objective view of the quality of the product, increases control, and reduces risk and cost. Based on the experience we’ve developed implementing some of the largest independent testing programs for the Federal government and CMMI® best practices, QSSI built an extensive Software Quality Assurance practice that manages requirements and quality with complete traceability from inception to completion."Right. QSSI, recall, is one of the HealthCare.gov prime contractors for the HIX rollout -- one now pointing fingers at everyone else. From their "Software Quality Assurance White Paper" (PDF) -
People and businesses rely on automated systems to deliver information quickly and accurately through the digital processing of complex tasks. As business requirements become increasingly intricate, systems begin to intersect and overlap themselves, increasing the systems’ complexity through the introduction of new factors and information. Now more than ever, we are moving towards an era of interconnectivity. By granting separate systems permission to shares utilities and information, we will be able to develop business intelligence and make connections that were previously unattainable. This level of computing is only sustainable through commitment to Software Quality Assurance (SQA). Organizations rely on developers to monitor and scrutinize the software engineering processes and methods used throughout the Software Development Life Cycle (SDLC) to develop their systems and assist them in the day-to-day operation of their business.
QSSI’s dedication to process improvement and standardized methods has directly impacted our ability to craft SQA solutions for our clients. As a CMMI® Level 3 organization, our standards and methodologies are well-defined and have been established over the course of our dynamic history. These standards and processes, coupled with the subject matter expertise gained through our provision of software development services to our clients, have cultivated an in-house SQA Practice Center that is comprised of best practices, expertise, techniques, supporting tools, and proven processes. Our ability to implement our SQA expertise into the SDLC assures that our clients’ needs are met and they can rely on the software we’ve worked with them to develop.These people are full of crap. Their "SQA" declarations are worthless. Marketing department platitudes, given their sorry performance on the HealthCare.gov initiative. There may well have been contract and political timeline inhibitions that led to their part in this mess, but they should have had the corporate courage to have blown the whistle prior to the launch. That they will likely be paid hundreds of millions of dollars anyway ought put everyone's hair on fire.
Full Life Cycle Testing
The goal of any system and its software is to deliver a solution to a targeted user group. In today’s competitive marketplace, it is essential that organizations are able to balance their ability to develop quality software and release that software in a timely fashion. Full Life Cycle Testing (FLC) is vital to those organizations that refuse to compromise on the quality of their product, yet remain driven to implement their solutions quickly.
QSSI Life Cycle Testing solutions expertly identify the necessary test activities essential to the success of the software and when the best time is for those activities to be executed. Our SQA Practice Center is the repository for our best practices and testing solutions that can be quickly tailored to meet the testing needs of our clients. Our deep understanding of the time-sensitive nature of testing inspired us to create a comprehensive testing approach that ensures requirements are explicitly defined and logically consistent throughout the Software Testing Life Cycle (STLC), and that the design code meets the established requirements.
BTW- I wonder how many people know that CSSI is now a subsidiary of United Health Group (specifically the OptumInsight part of the UHG org chart)?
HEADLINE JUST IN MY INBOX
Well, the hearing is over. Ended at 1:35 Eastern time. It was not as contentious as I thought it might be. Sebelius acquitted herself well, and bought herself some time, though if HHS misses its self-declared deadline for fixing HealthCare.gov, the calls for her head will reach deafening levels.
Interesting that she testified that CSSI has been given the new task of basically QA'ing their own work -- and will apparently be paid for it in addition to their existing contract. i.e., "Fee-For-Service (FFS)," like, say, when a hospital releases a patient only to have them re-admitted within a month, incurring new charges. CMS has vowed to quit paying for sucj re-admits, under "P4P" (Pay For Performance).
How comforting.
CODA
JAMA Forum: With a Bumpier Rollout Than Expected, Better Transparency Needed on Health Insurance ExchangesWell, yes, "transparency" would be nice. Including, say, transparency as to the relative natures of the bugs in the system. System bandwidth (including server inadequacy)? Code logic flaws (exacerbated by uncoordinated modular coding among various contractors)? "Fault tolerance"/error trapping inadequacies?
BY GAIL WILENSKY, PHD on OCTOBER 30, 2013
As we all now know, the start-up of the federally run insurance exchange websites and the first few weeks that the exchanges have been operating have been extremely bumpy—certainly bumpier than anyone (including me) had been predicting.
The experience of the District of Columbia and the 14 states that are running their own exchange websites has been mixed but generally better than that of the federal exchanges. Jeffrey Zients, the former senior person for management at the Office of Management and Budget who has been brought on to oversee the Obama Administration’s clean-up efforts, has publicly promised that the federal exchanges will be running smoothly for “most users” by the end of November.
A variety of reasons have been offered as to why the federal exchange website has been so dysfunctional—frequently crashing, sending repeat error messages partway through enrollment sequences, and so on. The administration initially attributed the problems to higher-than-anticipated volumes of users accessing the sites. Unfortunately, volume was, at most, only a contributing factor among many other problems. A statistic reported by Phil Galewitz of Kaiser Health News clearly characterized the early experiences: it took Galewitz 17 days and 63 attempts to enroll...
The concern is that with the difficulties encountered to date, the people most likely to doggedly persist through the process are the ones who need insurance the most—those who used to be in high-risk pools and others who know they need medical insurance because of their health needs. The worry is that the expected “low users” of health care—the “young immortals” or others who are otherwise healthy and likely low users—also need to sign up for insurance to get the risk pool at a manageable level. Whether they will be as persistent in making it through the enrollment process is unclear.
In the meantime, the federal government should take a lesson from the states and their willingness to share information about enrollees’ experiences in their exchanges. On the state exchange websites, it is easy to see how many people have visited, viewed options, set up accounts, and enrolled in private insurance or in Medicaid.
For reasons known only to the administration, the federal government has adamantly insisted it will not share information on actual private plan enrollment until at least mid-November. This type of continued stonewalling is a really dumb idea—not the least because it makes people wonder what else the government isn’t telling them.
Back in the 1980's I wrote apps in an environmental radiation lab in Oak Ridge, programs to be used in radionuclide contamination and dose exposure assay operations. Probably 90% or more of my code was devoted to "idiot trapping" -- i.e., making sure that lab techs couldn't enter incomplete or otherwise bad data via the user interfaces. The actual computational code -- the algebra -- was maybe 1% or less, with the remaining few percentages being devoted to results reporting output and RDBMS capture.How about data errors? I've not heard much at all these past two weeks about the extent to which bad data in the various distributed databases comprising the under-the-hood guts of HealthCare.gov have contributed to this fiasco. Your programming logic and module interfaces may be airtight, but you cannot code your way out of bad data already resident in your far-flung RDBMS -- other than to write expensive, laborious remediation code that goes through the data repositories and rectifies the ID'd and suspected errors in the tables ("data scrubbing"). Problematic, that idea.
I'll have some detailed thinking on that in my next post.
AT THE END OF THE DAY...
THIS IS FUNNY
___
More to come...